What is laryngitis?
Laryngitis describes inflammation of the vocal folds, regardless of the cause. As a result, it is what doctors call a non-specific term, or a somewhat generic diagnosis. In the case of hoarseness that comes with a sore throat, cough and a fever, and lasts just a few days, laryngitis is probably an adequate diagnosis, as most such cases are viral in origin and will resolve with rest, hydration and other routine measures. Under certain circumstances, antibiotics may be appropriate, as determined by your physician.
If the voice change does not resolve as expected along with the other symptoms of a cold or flu, a cause for the hoarseness must be determined. More than likely, it is not infectious, as the body’s immune system is equipped to react to this kind of infectious organism. The principal sources of chronic vocal fold irritation are acid reflux, allergies and cigarette smoke (secondhand included). It is also possible that a small irregularity of the vocal cord - like a polyp or a cyst - exists, and may not be noticeable without additional inflammation. This is sometimes the case in the person who notes that a cold “always goes to my vocal cords".
“Laryngitis” is sometimes used to explain persistent hoarseness. This is misguided not just because of the probable inaccuracy, but because hoarseness can be an early sign of a more serious problem. If there is a voice change that fails to improve for more than two to three weeks, the vocal folds themselves must be examined by a physician trained to do so. He or she should be able to give a more specific reason for the change and recommend treatment.
Laryngitis is not the same as hoarseness. When hoarseness persists beyond two weeks, especially without fever or other signs of illness, simple laryngitis is not an adequate diagnosis.
What are the symptoms of laryngitis?
Laryngitis generally produces hoarseness that gets worse with voice use. If the reason for the laryngitis is infectious, then there may also be fever and a sore throat, and perhaps a cough.
What does laryngitis look like?
The vocal folds have tiny blood vessels that enlarge with irritation or infection, producing a bloodshot look. They are commonly swollen, with a dull, rough appearance that replaces their typical satin sheen. With a lower-resolution endoscope, like a flexible fiberoptic tool, this may not be apparent, and the folds may simply look pink in place of their usual white.
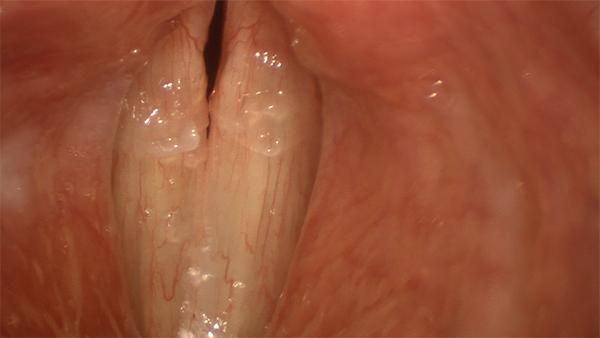
These vocal folds show signs of an early viral laryngitis, bloodshot in appearance with an excess of mucus.
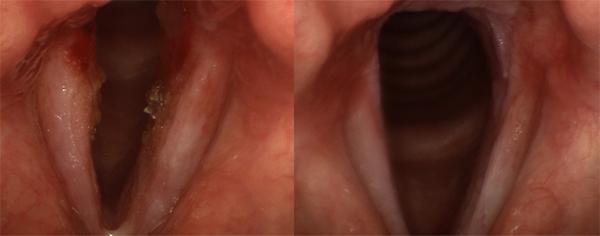
Before (left) and after (right) treatment views of a case of bacterial laryngitis. Initially, the vocal folds are swollen, with redness and crusting. Pus is visible at the bottom of the picture. After a course of antibiotics, some inflammation remains, but the infection is largely cleared.
How is laryngitis treated?
Initial measures to treat laryngitis are largely a matter of common sense - rest the voice and stay well hydrated. In most cases, this will be enough to shake off a viral infection. If there is a cough that produces a yellow or green colored sputum, or a coating in the back of the throat, there may be a bacterial infection that warrants antibiotics. Laryngitis that develops slowly, without fever, sore throat or other signs of infection, may represent irritation from other sources.
Most cases of laryngitis are treatable with medicine, and laryngitis by itself is not a reason for surgery.
It cannot be stressed enough that “laryngitis” is not an adequate diagnosis for hoarseness that goes on beyond two weeks. In such a case, the vocal cords must be examined to exclude another diagnosis. This is especially true in smokers, who have a high risk of laryngeal cancer.

