What is vocal fold hemorrhage?
“Hemorrhage” means bleeding. In the vocal fold, hemorrhage refers to bleeding into the superficial lamina propria, the layer that guarantees the pliability of the vocal fold for vibration (see Normal Voice Function). Because this layer is made up of a network of loosely-arranged fibers, blood spreads throughout it quickly, prohibiting the vocal fold from vibrating well. It does not take much blood to cause a vocal fold hemorrhage, and so this kind of bleeding is not a risk to overall health.
Hemorrhage is the result of phonotrauma, the physical stresses caused by voicing, upon the tiny blood vessels of the vocal fold. These may rupture and bleed after loud voicing, after sustained voicing, or when they are more fragile than normal, as when they are swollen during laryngitis. Small irregularities, like tiny polyps or weak areas in the blood vessel wall, called varices, also appear to predispose hemorrhage.
Hemorrhage may be a one-time occurrence, or it may recur. In situations of repeated bleeding, the vocal folds should be examined very carefully for the source of the bleeding.
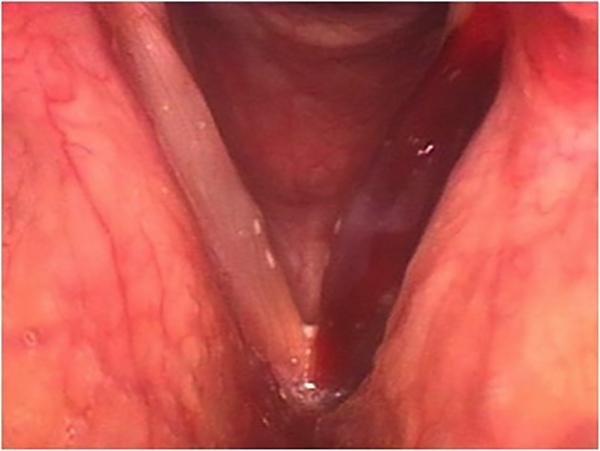
The whole left vocal fold (right in the image) has turned deep red from a hemorrhage.
What are the symptoms of vocal fold hemorrhage?
Hemorrhage causes hoarseness that usually develops over a very short period of time. It is typical for a hemorrhage to happen as a result of a specific event that required strenuous voice use, like a musical performance, or speaking over the noise at a party, or cheering at a baseball game. The hoarseness may be obvious in the speaking voice, or it can be subtler and cause only a change in the singing voice. There is no pain associated with a hemorrhage, and no difficulty swallowing or breathing.
What does vocal fold hemorrhage look like?
Because vocal fold hemorrhage takes place under the lining of the fold, blood has no way out, and spreads throughout the loose tissue layer of the superficial lamina propria. Blood can turn patches of the vocal fold red, or extend throughout the whole fold. Over time, as the blood resorbs, it undergoes the same changes as a bruise, turning darker red to brown and eventually fading. Repeated bleeding often leave a yellowish hue on the vocal folds, a byproduct of blood resorption. A small polyp or a dilated blood vessel, known as a varix, may sometimes be visible, and give a clue as to the reason for repeat hemorrhage.
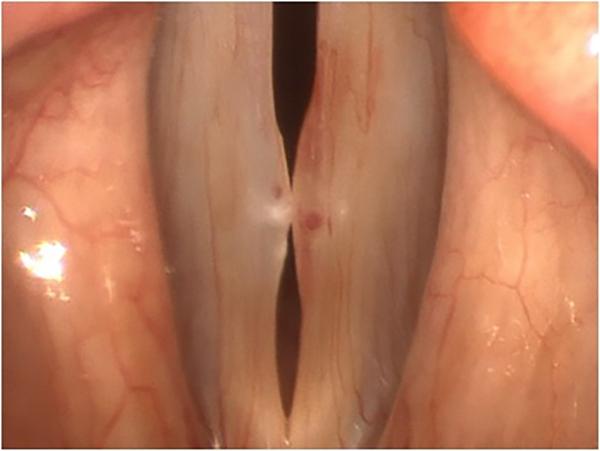
This image shows a resolving vocal fold hemorrhage on the left vocal fold (right in the image), visible as a darker blush of resorbing blood, in a patient with bilateral pseudocysts. A varix (the larger red dot), or dilated blood vessel, is visible in the pseudocyst and is likely the source of the bleeding.
How is vocal fold hemorrhage treated?
A hemorrhage that involves the entire vocal fold should be treated with immediate voice rest. Voice use should be limited or entirely suspended for several days. The exact length of time can be determined after repeat examinations. Steroids should not be used to “mask” the effects of a hemorrhage in order to press ahead with a performance - this is an invitation for further injury.
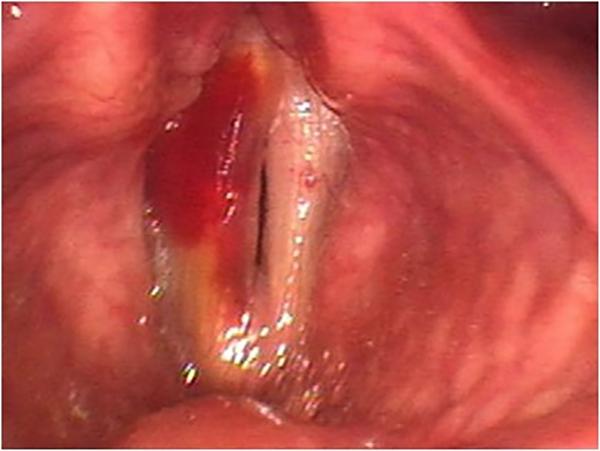
The woman whose throat is pictured above lost her voice after an amateur musical theater performance, one week before being seen. Her hemorrhage resolved entirely after adequate resting of her voice. She had no further difficulty.
Voice rest alone is adequate treatment for a single, isolated hemorrhage. Repeated hemorrhage, on the other hand, always has an underlying cause - be it a harmful voice behavior, or an irregularity on the vocal fold. In the first case, voice therapy may be useful, and in the second, microlaryngoscopy may be necessary to remove or repair any small irregularities or blood vessels prone to bleeding. This is among the more delicate surgeries in laryngology.

